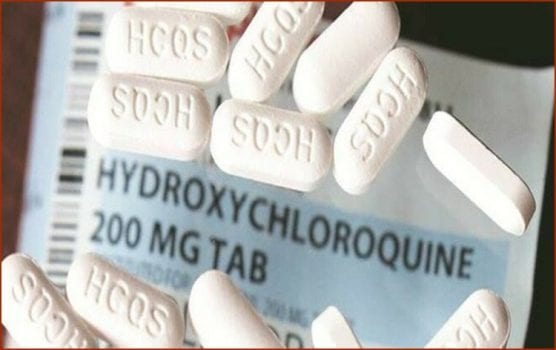
WASHINGTON — The largest study so far on using hydroxychloroquine to treat COVID-19 was published Friday in the Lancet: It found that patients showed no benefit and, worse, were more likely to die or develop an irregular heartbeat.
Funded by the William Harvey Distinguished Chair in Advanced Cardiovascular Medicine at Brigham and Women’s Hospital in Boston, the study involved 81,144 patients in the control group and 14,888 people in a treatment group. Most of the treatment group received hydroxychloroquine, either alone or with an antibiotic. Just over a third were treated with the related antimalarial drug chloroquine, either by itself or with an antibiotic.
Counting 10,698 deaths total, the study determined that “mortality was higher in the treatment groups compared with the control population.”
All combinations of protocols resulted in higher risk of death in the hospital or development of heart arrhythmia. Some 671 hospitals were included in the study, with data culled from six continents, covering patients who were hospitalized from mid-December to mid-April.
“Although generally safe when used for approved indications such as autoimmune disease or malaria, the safety and benefit of these treatment regiments are poorly evaluated in COVID-19,” according to the study, whose lead author is Dr. Mandeep Mehra, a heart specialist.
President Donald Trump, one of the more visible proponents of hydroxychloroquine to treat COVID-19, has yet to tweet any response. Just days earlier, he claimed during a press conference at the White House that he was taking the drug for “a couple of weeks,” despite warnings from the Food and Drug Administration suggesting high risk of mortality or irregular heartbeat when consumed outside of an approved medical or clinical setting.
A memo from White House physician Sean Conley was released the same day stating that he and the president had “numerous discussions” regarding the evidence for and against the use of hydroxychloroquine and concluded the potential benefit from treatment outweighed the relative risks. The memo did not state unequivocally that the president was currently on the regimen.
The 73-year-old president told reporters Tuesday, however, that he expected to finish taking the drug by Thursday.
“I’m not going to get hurt by it. It’s been around for 40 years for malaria and for lupus. I’m taking the two, the zinc and the hydroxy. So far I seem to be OK,” Trump said earlier this week.
Representatives for the White House did not immediately return a request for comment Friday.
The Lancet study considered factors such as a patient’s pre-existing health conditions like underlying lung disease and diabetes, as well as other issues like age, sex, race and even weight.
Last month, the American Heart Association, the American College of Cardiology and the Heart Rhythm Society issued guidance warning that the anti-malarial drug had serious implications for those patients who had underlying heart conditions.
That outlook has not changed, Mariell Jessup, chief science and medical officer for the American Heart Association, told Courthouse News.
“Mehra et al. observed increased risk of atrial fibrillation and ventricular tachycardia and a greater hazard for death among patients treated with chloroquine or hydroxychloroquine,” Jessup said, referring to the Brigham Young heart specialist behind Friday’s study in Lancet.
“These medications have increased cardiovascular toxicity, should not be administered outside of a clinical trial, and require close additional cardiovascular monitoring and treatment, as stated in our April 8 guidance,” Jessup continued.
As opposed to a randomized clinical trial, Friday’s study is observational — a term that the National Center for Biotechnology defines as those “in which the investigator makes no intervention and patients are allocated treatment based on clinical decisions.”
The center considers randomized, placebo-controlled clinical trials the gold standard for testing drug efficacy and risk, but says an observational study can be significantly useful when performed under rigorous standards.
“This study provides real-world evidence on the use of these therapeutic regiments by including a large number of patients from across the world. Thus, to our knowledge, these findings provide the most comprehensive evidence of the use of hydroxychloroquine and chloroquine (with or without a macrolide) for treatment of COVID-19,” the study in the Lancet concludes, using alternate terminology for an antibiotic.
Last month, researchers in Brazil published in the medical network JAMA that, of 81 patients ingesting chloroquine, those who took higher doses of the drug were roughly three times more like to die than those who took a smaller dose.
Frank Ruschitzka, who co-authored the Lancet study, said in a statement Friday that justifications for repurposing the antimalarial drug as a treatment for the novel coronavirus were based on a small number of anecdotal experiences.
“However, we now know from our study that the chance that these medications improve outcomes in Covid-19 is quite low,” said Ruschitzka, who is with the University Heart Center at University Hospital Zurich.
Since the novel coronavirus sprang up in Wuhan, China, last year, it has infected more than 5 million people worldwide. A case tracker at Johns Hopkins University says the United States leads the globe in confirmed deaths at 94,702. Though leading in deaths, the United States has the lowest mortality rate (6%) of the countries in the top 10. The United Kingdom, where 36,124 have died as of Friday, has a death rate of 14.3%.
— By Brandi Buchman
Like this:
Like Loading...
Related



 Tweet This
Tweet This Facebook
Facebook Digg This
Digg This Bookmark
Bookmark Stumble
Stumble RSS
RSS


























REAL NAMES ONLY: All posters must use their real individual or business name. This applies equally to Twitter account holders who use a nickname.
2 Comments
With Trump taking hydroxychloroquine, what are the odds he will end up having a heart issue? That is if he is telling the truth that he is taking it! Or was him telling the AMERICAN people he was using that drug a ploy to make him more money because he has stock or something in that manufacturing company overseas?
Very misleading propaganda. HXQ is a prophylactic treatment and NOBODY ever said it was a cure. It has protected many people.
This story is similar to reporting “new cases,” which is mostly useless information. Deaths-per-capita give us a better view of risk.
Some partisan, idiot so-called “journalists” want to blame Trump for anything and everything. It’s childish and very silly.