The Los Angeles County Department of Public Health confirmed Saturday 2,112 new cases of COVID-19 and 48 new deaths due to the virus countywide, and a total of 1,458 cases reported in the Santa Clarita Valley since the pandemic began, 152 more than reported Friday.
The high number of cases are, in part, due to a backlog of test results being processed and also a new lab beginning to report results in a timely manner through the county’s Electronic Laboratory Reporting (ELR) system.
To date, 20 people have died of the virus in the SCV — 16 resided in the city of Santa Clarita, 1 in Acton, 1 in Castaic, 1 in unincorporated Valencia and 2 in communities not yet named.
Countywide, Public Health has reported 53,651 positive cases of COVID-19 and a total of 2,338 deaths as of Saturday.
Ninety-three percent of people who died in L.A. County had underlying health conditions.
California Statewide Numbers
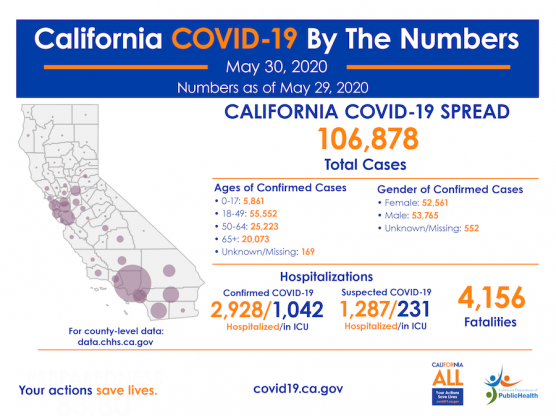
Statewide, California had 106,878 total confirmed cases and 4,156 deaths from COVID-19 as of May 29, the California Department of Public Health announced Saturday. There were 2,928 confirmed hospitalizations and 1,042 ICU hospitalizations.
Health Care Worker Infection Rates
As of May 29, local health departments have reported 9,910 confirmed positive cases in health care workers and 59 deaths statewide.
Santa Clarita Valley Saturday Update
Of the 1,458 cases reported to Public Health for the SCV to date, the community breakdown is as follows:
City of Santa Clarita: 754
Castaic: 572 (includes Pitchess Detention Center and North County Correctional Facility)
Canyon Country (unincorporated portion): 38
Stevenson Ranch: 34
Val Verde: 23
Acton: 11
Valencia (unincorporated portion west of I-5): 7
Agua Dulce: 9
Saugus (unincorporated portion): 4
Elizabeth Lake: 3
Bouquet Canyon: 1
Lake Hughes: 1
Newhall (Unincorporated portion): 1
Henry Mayo Saturday Update
Henry Mayo Newhall Hospital reported its 9th and 10th COVID-related deaths on Wednesday, both occurring in the last 36 hours, according to hospital spokesman Patrick Moody.
As of Wednesday, of the 1,555 persons tested at Henry Mayo to date, 208 tested positive, 1,289 were negative, 42 were pending and 9 patients were hospitalized in a dedicated unit receiving ICU-level care. A total of 73 COVID-19 patients have been discharged so far.
Discrepancies in the testing numbers are due to some patients being tested more than once, he said.
Ten of the SCV’s 20 fatalities to date have occurred at Henry Mayo, Moody confirmed Wednesday.
The hospital is now releasing numbers on a weekly basis (Wednesdays), unless there is a drastic change in the number of cases or a death has been confirmed, Moody said.
 Countywide, 36 people who died were over the age of 65 years old and eight people who died were between the ages of 41 and 65 years old. Thirty-three people had underlying health conditions including 26 people over the age of 65 years old, and seven people between the ages of 41 to 65 years old.
Countywide, 36 people who died were over the age of 65 years old and eight people who died were between the ages of 41 and 65 years old. Thirty-three people had underlying health conditions including 26 people over the age of 65 years old, and seven people between the ages of 41 to 65 years old.
Of those who died, information about race and ethnicity is available for 2,155 people (99 percent of the cases reported by Public Health); 40% of deaths occurred among Latino/Latinx residents, 28% among White residents, 18% among Asian residents, 12% among African American residents, 1% among Native Hawaiian/Pacific Islander residents and 1% among residents identifying with other races. Upon further investigation, 23 cases reported earlier were not L.A. County residents. As of today, 6,486 people who tested positive for COVID-19 (13% of positive cases) have been hospitalized at some point during their illness. There are 1,415 people who are currently hospitalized, 28% of these people are in the ICU and 19% are on ventilators. Testing capacity continues to increase in L.A. County, with testing results available for over 580,000 individuals and 8% of people testing positive.
Public Health continues to track health outcomes by race, ethnicity and income level data of people who have been tested, hospitalized and died from COVID-19. African Americans, Native Hawaiian/Pacific Islanders, and people living in communities with high levels of poverty continue to have the highest rate of death per 100,000 people for COVID-19 when compared to other groups. Native Hawaiian/Pacific Islanders have a death rate of 99 per 100,000, African Americans have a death of 29 per 100,000, Latinos/Latinxs have a death of 26 per 100,000, Asians have a death rate of 19 per 100,000, and Whites have a death rate of 14 per 100,000. People who live in areas with high rates of poverty have almost four times the rate of deaths for COVID-19 with 46 per 100,000 people, compared with communities with very low poverty levels who had a death rate of 12 per 100,000. Public Health continues collaboration with community, healthcare, and philanthropic partners to improve testing, connection to care and services, and in-language and culturally appropriate communications to the communities experiencing these inequitable outcomes.
“Each day, we join with families and friends mourning the devastating loss of life to COVID-19 and we keep those who are grieving in our thoughts and prayers,” said Barbara Ferrer, PhD, MPH, MEd, Director of Public Health. “L.A. County is on our recovery journey, and as more businesses and spaces re-open, it has never been more important – as individuals, businesses and institutions – to use the tools that we all have to take care of each other and to continue to slow the spread of COVID-19. This means practicing physical distancing, wearing cloth face coverings when in public, and adhering to all directives in the Health Officer order.”
Los Angeles County received approval by the State on its variance. This variance allows the County to move through Stage 2 of the State’s 4-stage Pandemic Roadmap at an accelerated rate as determined by our local Health Officer. Public Health has amended the current Health Officer Order, Safer at Work and in the Community, to allow in-person dining at restaurants and hair salons to reopen once the establishments are able to implement the required distancing and infection control directives. The directives are contained in sector-specific protocols that guide re-opening and are available online. Inspectors will continue to offer technical assistance as they monitor businesses for compliance with the Health Officer Order. Higher-risk businesses remain closed.
As the recovery journey continues, more people being around one another may result in more transmission of COVID-19, more cases, and more hospitalizations and deaths. The actions everyone takes today will be reflected in our metrics in two or three weeks. Everyone must continue to follow distancing and infection control directives and wear a clean cloth face covering that securely covers both your nose and mouth when in contact with other people not in your household. Public Health will assess the activities allowed by the Order on an ongoing basis. L.A. County is in stage two of the five-stage Roadmap to Recovery and until the final stage five is reached, Health Officer Orders and directives will continue to ensure that we slow spread of COVID-19 to prevent an overwhelming surge of COVID-19 cases at healthcare facilities.
The Reopening Protocols, COVID-19 Surveillance Interactive Dashboard, Roadmap to Recovery, Recovery Dashboard, and additional things you can do to protect yourself, your family and your community are on the Public Health website, www.publichealth.lacounty.gov.
The best protection against COVID-19 continues to be to wash your hands frequently, avoid touching your eyes, nose, and mouth with unwashed hands, self-isolate if you are sick, practice physical distancing, and wear a clean face covering when in contact with others from outside your household. People who have underlying health conditions remain at much greater risk for serious illness from COVID-19, so it will continue to be very important for the County’s vulnerable residents to stay at home as much as possible, to have groceries and medicine delivered, and to call their providers immediately if they have even mild symptoms.
More from California Saturday
As testing capacity continues to increase across the state, the California Department of Public Health is working to expand access to COVID-19 testing. Testing should be used for medical evaluation of persons with symptoms of COVID-19 as well as for efforts by public health agencies and essential employers to prevent and control the spread of COVID-19.
– Hospitalized patients
– Symptomatic and asymptomatic healthcare workers, first responders, and other social service employees
– Symptomatic individuals age 65 and older or symptomatic individuals of any age with chronic medical conditions that increase the risk of severe COVID-19 illness
– Individuals who are tested as part of disease control efforts in high-risk settings
– Asymptomatic residents and employees of congregate living facilities when needed to prevent disease transmission
– Symptomatic and asymptomatic individuals in essential occupations such as grocery store and food supply workers, utility workers and public employees
– Other individuals with symptoms consistent with COVID-19
As of May 29, 1,888,595 tests have been conducted in California and reported to the California Department of Public Health. This represents an increase of 53,117 tests over the prior 24-hour reporting period. These numbers include data from commercial, private and academic labs, including Quest, LabCorp, Kaiser, University of California and Stanford, and the 25 state and county health labs currently testing.
California Demographics/Racial Demographics – A More Complete Picture
The California Department of Public Health is committed to health equity and collecting more detailed racial and ethnic data that will provide additional understanding for determining future action. Health outcomes are affected by forces including structural racism, poverty and the disproportionate prevalence of underlying conditions such as asthma and heart disease among Latinos and African American Californians. Only by looking at the full picture can we understand how to ensure the best outcomes for all Californians.
The differences in health outcomes related to COVID-19 are most stark in COVID-19 deaths. We have nearly complete data on race and ethnicity for COVID-19 deaths, and we are seeing the following trends. Overall, for adults 18 and older, Latinos, African Americans and Native Hawaiians and Pacific Islanders are dying at disproportionately higher levels. The proportion of COVID-19 deaths in African Americans is about double their population representation across all adult age categories. For Native Hawaiians and Pacific Islanders, overall numbers are low, but about three-fold difference between the proportion of COVID-19 deaths and their population representation. More males are dying from COVID-19 than females, in line with national trends.
More information is available at COVID-19 Race and Ethnicity Data.
Your Actions Save Lives
Every person has a role to play. Protecting yourself and your family comes down to common sense:
– Staying home except for essential needs/activities.
– Practicing social distancing.
– Washing hands with soap and water for a minimum of 20 seconds.
– Avoiding touching eyes, nose or mouth with unwashed hands.
– Covering a cough or sneeze with your sleeve, or disposable tissue. Wash your hands afterward.
– Avoiding close contact with people who are sick.
– Staying away from work, school or other people if you become sick with respiratory symptoms like fever and cough.
– Following guidance from public health officials.
What to Do if You Think You’re Sick
Call ahead: If you are experiencing symptoms of COVID-19 (fever, cough or shortness of breath) and may have had contact with a person with COVID-19, or recently traveled to countries with apparent community spread, call your health care provider before seeking medical care so that appropriate precautions can be taken.
For more information about what Californians can do to prevent the spread of COVID-19, visit Coronavirus (COVID-19) in California.
California continues to issue guidance on preparing and protecting California from COVID-19. Visit Coronavirus (COVID-19) in alifornia and California Department of Public Health COVID-19 Guidance.
Always check with trusted sources for the latest accurate information about novel coronavirus:
– Los Angeles County Department of Public Health
– California Department of Public Health
– Centers for Disease Control and Prevention
– Spanish
– World Health Organization
L.A. County residents can also call 2-1-1.
Like this:
Like Loading...
Related



 Tweet This
Tweet This Facebook
Facebook Digg This
Digg This Bookmark
Bookmark Stumble
Stumble RSS
RSS


























REAL NAMES ONLY: All posters must use their real individual or business name. This applies equally to Twitter account holders who use a nickname.
0 Comments
You can be the first one to leave a comment.